Knee injuries can often occur during sports or recreational activities, but other knee issues can happen in the course of everyday work or due to disease. Whether your knee pain is due to an injury or a chronic condition, OAM specialists work to successfully diagnose and treat your knee concerns, returning you to as much pain-free activity as soon as possible. Treatment options vary by patient, severity of injury, and diagnosis. Conservative options such as rest, pain medication, and physical therapy should always be investigated. Other common knee treatments include injections or surgery, if needed.
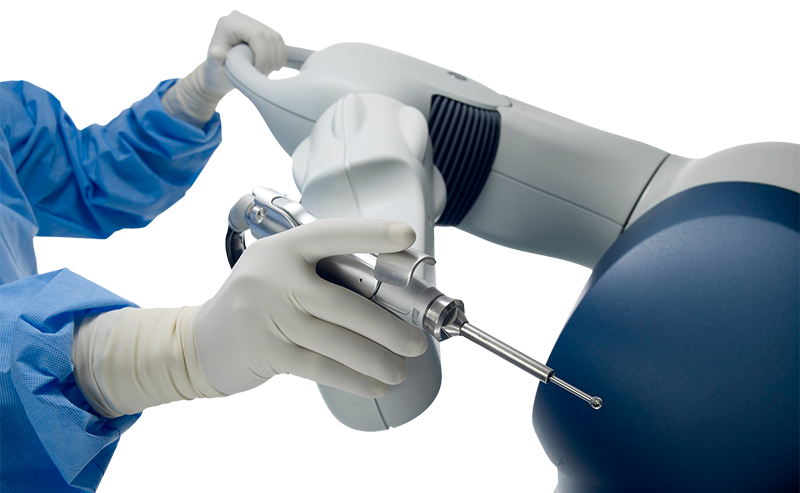
OAM also offers joint replacement using the Mako Robotic-Arm Assisted Surgery System. OAM has surgeons that are trained and certified to perform robotic-arm assisted partial knee and total knee replacement procedures using Stryker’s Mako System.
To help educate our patients and prepare them for before, during, and after surgery, we have created an informative video. If you are scheduled for total joint replacement surgery or are considering it in the future, please click the link below to watch the video.
The anterior cruciate ligament (ACL) is a ligament on the inside of the knee joint that connects the tibia to the femur. The function of the ACL is to prevent the tibia from shifting forward on the femur.
ACL injuries are common during sports activities. Often, tears result from a non-contact twisting injury. Sports such as soccer and football are especially high risk. Female athletes are three to four times more likely to suffer an ACL injury than males. Unfortunately, the ACL rarely heals on it's own. Because the healing potential of the ACL is low, repair of the damaged ligament is often not possible. In older individuals, a torn ACL can sometimes be treated non-surgically. In young, active patients surgery is typically recommended to reconstruct the injured ACL. This can be done arthroscopically as an outpatient in most cases. The most common options to reconstruct the ACL are to use the middle third of the patellar tendon, the hamstring tendons, or a cadaver tendon. All of the reconstruction options have pluses and minuses, and this is something your surgeon can discuss.
Potential complications of surgery include knee stiffness, infection, DVT, and retear of the new ACL. Fortunately, retear of the ACL is not common, occurring in approximately 5-10 percent of cases. After surgery, patients are typically in a brace for several weeks. Physical therapy starts several days after surgery and will likely continue for several months. Typical time to return to sports activities is six to eight months.
For additional information about this condition, we have included this complete patient eduction sheet as a pdf to view, download and print:
Injury to the knee can cause damage to the articular lining cartilage in the knee joint, or sometimes to both the cartilage and the bone.
If the injury is restricted to the cartilage, it will not show up in a plain X-ray; it may be noted on an MRI. An arthroscopy (using a special instrument to look inside the joint) can thoroughly identify it.
If a piece of cartilage or bone has become detached in the knee and the injury is not treated immediately, the loose part can 'swim around' in the joint. This means that it may occasionally get stuck, causing pain and a feeling that the knee is locked. The knee may also click and swell up. Such a condition is called a loose body in the knee.
As cartilage does not show up on an X-ray, the loose body will only be visible if it consists of bone.
Arthritis simply means an inflammation of a joint causing pain, swelling, stiffness, instability and often deformity. Severe arthritis interferes with a person’s activities and limits his or her lifestyle.
Osteoarthritis or Degenerative Joint Disease is the most common type of arthritis. Osteoarthritis is also known as "wear and tear arthritis" since the cartilage simply wears out. When cartilage wears away, bone rubs on bone causing severe pain and disability. The most frequent reason for osteoarthritis is genetic, since the durability of each individual’s cartilage is based on genetics. If your parents have arthritis, you may also get it.
Trauma can also lead to osteoarthritis. A bad fall or blow to the knee can injure the joint. If the injury does not heal properly, extra force may be placed on the joint, which over time can cause the cartilage to wear away.
Inflammatory Arthritis Swelling and heat (inflammation) of the joint lining causes a release of enzymes which soften and eventually destroy the cartilage. Rheumatoid arthritis, Lupus and psoriatic arthritis are inflammatory in nature.
For additional information about this condition, we have included this complete patient eduction sheet as a pdf to view, download and print:
The lateral collateral ligament (LCL) is one of the four knee ligaments. It spans the distance from the end of the femur (thigh bone) to the top of the fibula (thin, outer, lower leg bone) and is on the outside of the knee. The lateral collateral ligament resists widening of the outside of the joint. A lateral collateral ligament injury happens from a direct force from the side of the knee, causing moderate to severe knee pain and ligament injury which often leads to knee surgery. It is a much less common ligament injury than the medial collateral ligament (MCL) but commonly occurs with another ligament injury to the knee.
Your knee is the largest joint in your body and one of the most complex. Because you use it so much, it is vulnerable to injury. Because it is made up of so many parts, many different things can go wrong.
Meniscal tears are among the most common knee injuries. Athletes, particularly those who play contact sports, are at risk for meniscal tears. However, anyone at any age can tear a meniscus. When people talk about torn cartilage in the knee, they are usually referring to a torn meniscus.
Two wedge-shaped pieces of cartilage (meniscus) act as "shock absorbers" be-tween your thighbone (femur) and shinbone (tibia). They are tough and rubbery to help cushion the joint.
Common tears include longitudinal, parrot-beak, flap, bucket handle, and mixed/complex. Sports-related meniscal tears often occur along with other knee injuries, such as anterior cruciate ligament tears.
Sudden meniscal tears often happen during physical activity. An individual may squat and twist the knee, causing a tear. Direct contact, like a tackle, is sometimes involved.
Older people are more likely to have degenerative meniscal tears. Cartilage weakens and wears thin over time. Aged, worn tissue is more prone to tears. An awkward twist when get-ting up from a chair may be enough to cause a tear, if the menisci have weakened with age.
You might feel a "pop" when you tear a meniscus. Most people can still walk on their injured knee. Many athletes keep playing with a tear. Over 2 to 3 days, your knee will gradually be-come more stiff and swollen.
The most common symptoms of meniscal tear are:
Without treatment, a piece of meniscus may come loose and drift into the joint. This can cause your knee to slip, pop or lock.
For additional information this condition, we have included this complete patient eduction sheet as a pdf to view, download and print:
As long as your kneecap (patella) stays in its groove in the knee, you can walk, run, sit, stand, and move easily. When the kneecap slips out of the groove, problems and pain often result.
The kneecap connects the muscles in the front of the thigh to the shinbone (tibia). As you bend or straighten your leg, the kneecap is pulled up or down. The thighbone (femur) has a V-shaped notch (femoral groove) at one end to accommodate the moving kneecap. In a normal knee, the kneecap fits nicely in the groove.
If the groove is uneven or too shallow, the kneecap could slide off, resulting in a partial or complete dislocation. Loose ligaments on one side of the kneecap or over-tight ligaments on the other can also cause instability. Additionally, a sharp blow to the kneecap, as in a fall, could also pop the kneecap out of place.
For additional information about this condition, we have included this complete patient eduction sheet as a pdf to view, download and print:
Arthritis of the knee is a leading cause of disability in the United States. Patellofemoral arthritis affects your kneecap (patella bone). It causes pain in the front of your knee and can make it difficult to kneel and climb stairs.
The patella is a small bone located in front of your knee joint — where the thighbone (femur) and shinbone (tibia) meet. It protects your knee and connects the muscles in the front of your thigh to your tibia.
The patella rests in a groove on top of the femur called the trochlear groove. When you bend and straighten your knee, the patella moves back and forth inside the groove.
The ends of the femur, trochlear groove, and the under-sides of the patella are covered with a slippery substance called articular cartilage. This helps the bones glide smoothly along each other as you move your leg.
Patellofemoral arthritis occurs when the articular cartilage along the trochlear groove and on the underside of the patella wears down and becomes inflamed. When cartilage wears away, it becomes frayed, and when the wear is severe, the underlying bone may become exposed. Moving the bones along this rough surface is painful.
The main symptom of patellofemoral arthritis is pain. Because the patellofemoral joint is in front of the knee, you may have pain in this area. The pain can be present at rest or with no activity at all. Most of the time, however, it is brought on by activities which put pressure on the kneecap, such as kneeling, squatting, climbing stairs, and getting up from a low chair.
You may also experience a crackling sensation called crepitus when you move your knee. Crepitus is sometimes painful and can be loud enough for others to hear. When the disease is advanced, your kneecap may get stuck or "catch" when you straighten your knee.
For additional information this condition, we have included this complete patient eduction sheet as a pdf to view, download and print:
Runners, jumpers, and other athletes such as skiers, cyclists, and soccer players put heavy stress on their knees. Runner’s knee is a term used to refer to a number of medical conditions that cause pain around the front of the knee (patellofemoral pain). These conditions include anterior knee pain syndrome, patellofemoral malalignment, and chondromalacia patella
The knee is a complex structure. A number of factors can contribute to runner’s knee:
Patellofemoral pain may be the result of irritation of the soft tissues around the front of the knee. Strained tendons are fairly common in athletes. Other contributing factors to patellofemoral pain include overuse, muscle imbalance and inadequate stretching. Pain that begins in another part of the body, such as the back or hip, may cause pain in the knee (referred pain).
In some people with runner’s knee, the kneecap is often out of alignment. If so, vigorous activities can cause excessive stress and wear on the cartilage of the kneecap. This can lead to softening and breakdown of the cartilage on the patella (chondromalacia patella) and cause pain in the underlying bone and irritation of the joint lining.
A dull, aching pain under or around the front of the kneecap (patella) where it connects with the lower end of the thighbone (femur). Pain occurs when walking up or down stairs, kneeling, squatting, and sitting with a bent knee for a long period of time.
Patient Education Sheets
For additional information about this condition, we have included this complete patient eduction sheet as a pdf to view, download and print:
The four ligaments that stabilize the knee are:
The PCL has been described as one of the main stabilizers of the knee. It is broader and stronger than the ACL. It connects the femur (thigh bone) to the tibia (shin bone). Its function is to prevent the posterior translation of the tibia relative to the femur.
It has been reported that there is only a 2% incidence of isolated PCL tears. PCL injury commonly occurs in sports such as football, soccer, basketball, and skiing. A forceful hyperextention of the knee or a direct blow just below the knee cap will disrupt the PCL and cause knee pain and PCL Injury. For example, the football player who is tackled with a direct hit to the knee will hyperextend the limb and sustain a PCL Injury. The basketball player who lands on the court directly on a bent knee will tear his PCL resulting in knee pain. A thorough evaluation by a sports medicine specialist is needed to assess the extent of the ligament injury and the appropriate treatment options. Both examples frequently lead to knee pain which often requires knee surgery.
Plumbers, carpet layers, and other people who spend a lot of time on their knees often experience swelling in the front of the knee. The constant friction irritates a small lubricating sac (bursa) located just in front of the kneecap (patella). The bursa enables the kneecap to move smoothly under the skin. If the bursa becomes inflamed, it fills with fluid and causes swelling at the top of the knee. This condition is called kneecap (prepatellar) bursitis.
For additional information about this condition, we have included this complete patient eduction sheet as a pdf to view, download and print:
The medial collateral ligament (MCL) is one of four ligaments that are critical to the stability of the knee joint. A ligament is made of tough fibrous material and functions to control excessive motion by limiting joint mobility. The four major stabilizing ligaments of the knee are the anterior and posterior cruciate ligaments (ACL and PCL, respectively), and the medial and lateral collateral ligaments (MCL and LCL, respectively).
The MCL spans the distance from the end of the femur (thigh bone) to the top of the tibia (shin bone) and is on the inside of the knee joint. The medial collateral ligament resists widening of the inside of the joint, or prevents "opening-up" of the knee.
This is an incomplete tear of the MCL. The tendon is still in continuity, and the symptoms are usually minimal. Patients usually complain of pain with pressure on the MCL, and may be able to return to their sport very quickly. Most athletes miss 2-4 weeks of play.
Grade II injuries are also considered incomplete tears of the MCL. These patients may complain of instability when attempting to cut or pivot. The pain and swelling is more significant, and usually a period of 4-6 weeks of rest is necessary.
A grade III injury is a complete tear of the MCL. Patients have significant pain and swelling, and often have difficulty bending the knee. Instability, or giving out, is a common finding with grade III MCL tears. A knee brace or a knee immobilizer is usually needed for comfort, and healing may take 6 weeks or longer.
For additional information this condition, we have included this complete patient eduction sheet as a pdf to view, download and print:
The meniscus is a very important shock absorber of the knee made of a very strong substance called fibrocartilage. It protects the cartilage of the joint, keeping it from wearing out and causing early arthritis. A large percentage of our body weight is distributed through the meniscus as we walk, run, and jump. The meniscus adds to the stability of the knee joint by helping the shape of the femur or thigh bone conform to the tibia or leg bone. The meniscus also plays a role in the nourishment of the joint cartilage that covers the bones in the joint.
An acute meniscal tear may be heard as a "pop" and felt as a tear or rip in the knee. Many are followed within a few minutes to hours by swelling of the knee as a result of blood accumulation. Some do not result in much swelling and some present themselves in a less acute fashion. Patients with meniscal tears often describe a popping or catching in their knee. Some actually can feel something out of place. In the most dramatic situations the knee will actually lock, preventing the patient from fully extending or straightening the knee -- or occasionally from flexing or bending it. The pain or discomfort is usually along the joint line or where the femur and tibia bone come together. It often starts out relatively painful; then with time, much (if not all) of the pain disappears except with certain activities. Some patients will have the tear become asymptomatic (no symptoms) for a time, especially if their activity level decreases significantly.
Several events can cause the meniscus to become damaged. It can tear or rip from force, pinching it between the femur and the tibia. Most frequently this is a twisting-type force and is relatively common in sports-related knee injuries. Occasionally it is associated with a ligament rupture. It does not always require a major fall or twist to cause a meniscal tear. Some occur with nothing more than getting up from a squatting position. Certain meniscal tears occur gradually over a long period of time. In older patients these may represent so-called degenerative meniscal tears and may not be symptomatic. The location of the tear within the meniscus may determine the type of treatment which is most appropriate.
For additional information about this condition, we have included this complete patient eduction sheet as a pdf to view, download and print:
Injuries can happen anytime so we have immediate appointments available at our Muskegon office. Our orthopaedic urgent care is open to accommodate same day visits for the evaluation of knee injuries.